This article includes graphic scenes of injury and death.
As soon as he arrived on the scene, Bashar – a first responder with the Syrian Civil Defense or White Helmets – knew that this attack was unlike anything he had ever encountered.
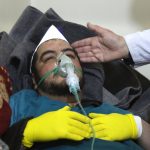
“Normally when we go to a strike location, there are body parts scattered and blood,” Bashar told Physicians for Human Rights (PHR). We’re withholding his full name to protect his identity. But this time he saw people without clear injuries writhing on the ground. “Their eyes were turning white. They were foaming from the mouth and convulsing. It looked like people were struggling against death. They were resisting death.”
On April 4, just before daybreak, Syrian government aircraft launched an assault on the town of Khan Sheikhoun in an opposition-held area of Idlib province. The payload included a chemical agent, reportedly sarin – among the most deadly toxins in existence. It is colorless, odorless, and tasteless, and its use is banned under international law.
Bashar was one of a group of health professionals PHR interviewed in the hours and days after the attack. For more than six years, health professionals have been on the front lines of some of the most gruesome war crimes committed in Syria. As PHR has documented, both medical facilities and personnel have come under relentless fire – we’ve counted 454 attacks on 310 separate facilities as well as the deaths of 796 medical personnel as of October 2016.
The testimony of Bashar and his colleagues – along with a medical and forensic analysis of photos and videos – paints a vivid picture of the chaotic, terrifying hours that followed the Khan Sheihkoun attack. And it contributed to PHR’s conclusion that a chemical compound like sarin – a deadly material whose use in warfare is universally banned – was unleashed on a residential neighborhood of a small Syrian town.
GRAPHIC FOOTAGE In their review of this footage, PHR medical experts concurred that people appeared to show oral and nasal secretions and frothing, agonal (gasping) breathing, and severe respiratory distress — symptoms consistent with exposure to a nerve agent such as sarin.
Bashar was one of the first to tend to victims in Khan Sheikhoun. With limited supplies, he began loading patients into his vehicle to take them to the nearest clinic. He could only drive a short distance before his vision began to blur. He told PHR he felt “an indescribable exhaustion as if I hadn’t slept in a year.” Before losing consciousness, he radioed his colleagues to transport his patients to the nearest medical facility. He awoke later that evening but is still recovering from nerve damage.
“To definitively prove the evidence of a particular chemical agent, you need biological or environmental samples,” said PHR’s director of programs, Dr. Homer Venters. He was part of PHR’s medical review team that concluded a chemical agent was used in Khan Sheikhoun. “But observing patients and interviewing doctors and first responders can help narrow likely causes. In this case, we could clearly see symptoms like foaming at the mouth, dilated pupils, and respiratory distress – symptoms that, taken together, and without indications of other trauma, are consistent with exposure to an organophosphate like sarin.”
Health professionals interviewed by PHR said they encountered similar symptoms as patients began streaming into their emergency wards. Hazem, a nurse whose full name we’re withholding to protect his identity, said he and his colleagues took precautions to protect themselves and prevent further exposure.
“First we had to undress the patients and wash them. We provided them with atropine, cortisone, and oxygen,” he told PHR. “We are under-equipped and were unprepared for an attack of such scale.”
GRAPHIC FOOTAGE PHR medical experts reviewed footage showing multiple patients with respiratory distress. Those experts agreed that, in the absence of other traumatic injury, those patients had likely been exposed to a nerve agent like sarin.
Hazem and his colleagues did their best to provide initial treatment, but, for more urgent cases, they needed to send patients to other nearby facilities that were better equipped. As fighting in Idlib province has intensified in recent weeks, hospitals in the region have been attacked repeatedly, and life-saving drugs and equipment are in short supply. The week before the Khan Sheikhoun attack, PHR documented two strikes on medical facilities in nearby Hama province.
Dr. Zakariya, an orthopedic surgeon at the Khan Sheikhoun hospital who asked that we not use his real name, also scrambled to see as many patients as possible. “I treated more than 50 patients,” he told PHR. “And I saw ten people who died.” Dr. Zakariya was overwhelmed by the fact that the chemical strike took place in a largely residential neighborhood of the town, meaning that many of the victims were related to one another. Around midday, as he and his colleagues offered whatever treatment they could, the hospital shook. It had come under fire.
“The hospital was targeted while I was in surgery treating an injured person from another strike,” said Dr. Zakariya, who nevertheless continued operating. “After we completed the surgery, the hospital was targeted by yet another airstrike that rendered the hospital out of service. The hospital has been closed ever since.”
GRAPHIC FOOTAGE Video inside the Khan Sheikhoun hospital after an airstrike targeted the facility. The clinic — built into a cave for protection — was treating patients from the April 4 chemical strike when the attack took place.
The hospital staff are still working to restore the facility, an increasingly urgent task as fighting nearby escalates. One of the hospital’s board members told PHR that he and his staff are stretched to their limits. “The medical staff live under indescribable circumstances,” he told PHR. “Sometimes we cannot go home or see our families for weeks. We are exposed to great risks. There is no safety for us and no comfort.”